IDAHO — As of Thursday afternoon, there were over 16,000 positive COVID-19 cases in Idaho that have not been processed by local public health districts.
This delay is causing the state’s data dashboard to not exactly reflect how many new cases are reported in the state each day.
The over 16,000 positive laboratory cases are pending local public health district review and follow-up where disease investigators verify the person’s residence in Idaho and ask them about their symptoms.
As soon as they are done confirming their Idaho residency, the state is notified and the case is submitted to the state to be added to the daily cases count, but due to the increase of cases, the process has slowed down.
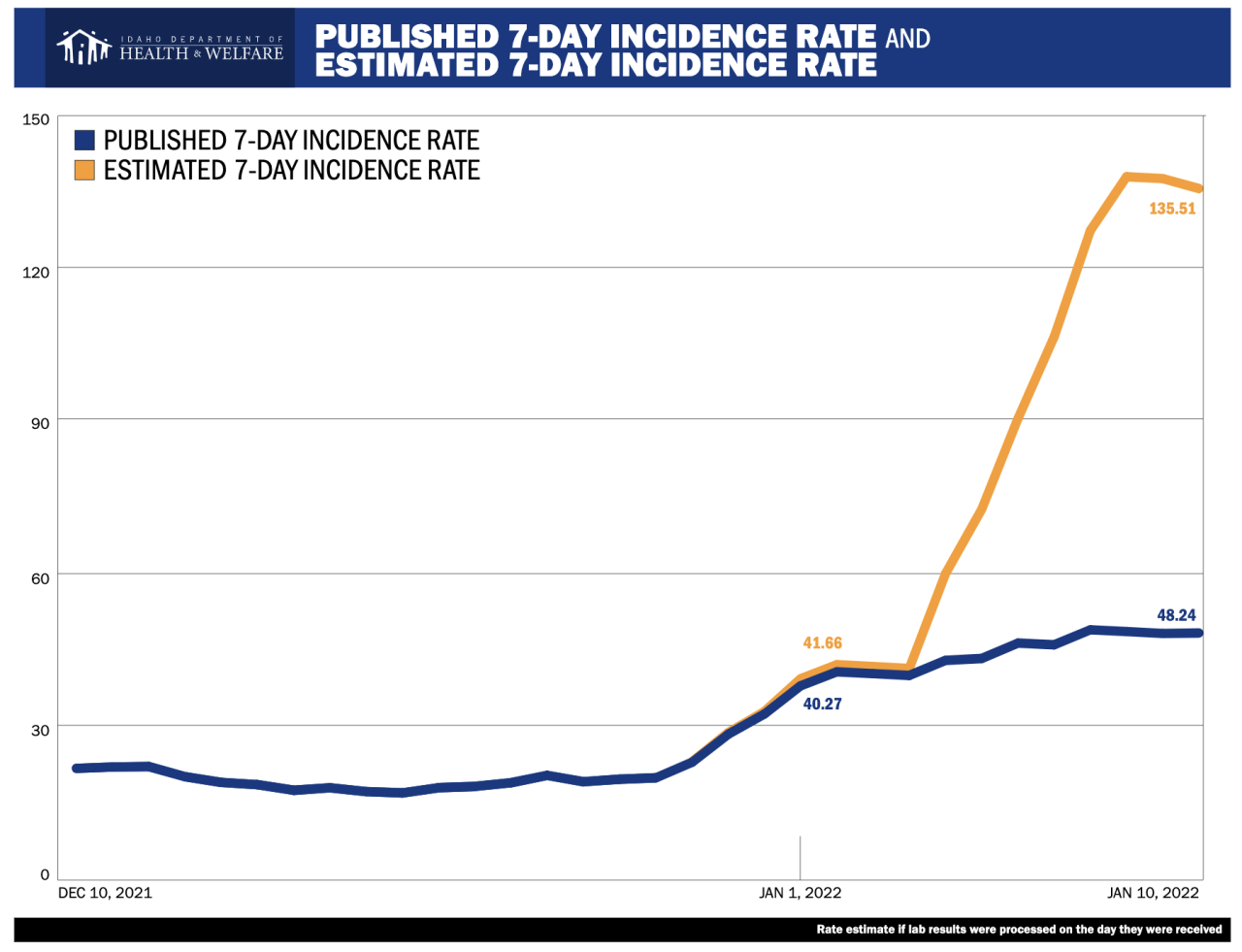
“With about 3,000 positive results that Idaho public health districts are having to manage every day, it is exceedingly difficult to turn those investigations around in 24 hours and for that reason, some of our public health districts have been unable to keep up with the recent volume of laboratory results,” Deputy State Epidemiologist Kathryn Turner said.
Health officials say currently, the stress and strain on hospitals and health care systems is because more staff are out sick.
Related: COVID-19 in Idaho: 2 lawmakers test positive, Caldwell School District announces closure
“We are concerned that people may have even a false sense of assurance, that our data doesn’t look too bad if they’re not realizing how many of our laboratory reports are yet unprocessed,” State Epidemiologist Christine Hahn said. “We are not immune from this omicron wave. We are seeing rising case numbers that continue to increase and we expect to see increasing hospitalizations in the coming days and weeks.”
On a media briefing Tuesday, the Department of Health and Welfare director Dave Jeppesen said it would not surprise him if the state went back into Crisis Standards of Care, but this time, it would most likely be driven by staffing shortages rather than an increase in hospitalizations.
A recording of today's media briefing on COVID-19 is now available: https://t.co/ANlitcHogz
— DHW (@IDHW) January 11, 2022




